Premature Babies
When to start solids and what to expect.
Contents
- When Should a Premature Baby Start Solids?
- Look for Readiness Signs (Not Just Dates)
- Baby not sitting upright?
- What About Iron?
- If Your Baby Has Additional Feeding Needs
- Baby-Led Weaning or Puree for Premature Babies?
- Feeding as a Sensory Experience
- Feeding Challenges
- When to seek extra support:
- Other Common Concerns
- Key Takeaways

Back in stock
Toddler to Table now back in stock!
Your guide to bringing the family together, one meal (and delicious recipe) at a time.
Order nowWhen Should a Premature Baby Start Solids?
For babies born prematurely, the timing for starting solids can look a little different.
Some preterm babies may be ready closer to 6 months chronological age (the age from birth), while others may need more time – sometimes closer to 6 months corrected/adjusted age (the age they would be if born on their due date).
Chronological Age vs Adjusted Age
- Chronological age is your baby’s age from birth.
- Adjusted (corrected) age is how old your baby would be if they were born on their due date (chronological age minus the number of weeks your baby was born early).
Example:
If your baby was born at 32 weeks (8 weeks early) and is now 6 months old from birth, their adjusted age is 4 months – and feeding readiness will likely align more closely with 4 months.We usually use adjusted age for developmental milestones, including feeding, until around 2 years of age. In reality, many preterm babies develop somewhere between their chronological and adjusted ages.
Look for Readiness Signs (Not Just Dates)
You can begin offering solids once your baby shows all of these signs:
- Sitting: Can sit upright with little or no support.
Now this can get a bit confusing – what is sitting unassisted? The aim is that whilst they may still topple a little bit, that they can support themselves in a seated position for a period of time once in the highchair or on your lap. Read more here.
- Head control: Holds head steady and upright without ‘bobbing’
Their head shouldn’t be ‘bobbing’ around or slumping forward. This is very important from a safety point of view, because if their head is slumped then this can occlude the airway and increase the risk of choking.
Having strong head and neck control also helps them to turn their head towards or away from food to indicate if they have had enough food or want more food.
- Hand-to-mouth skills: Can reach for objects and bring them to the mouth
- Interest in food: Watches you eat, leans forward, opens mouth, or reaches for food
Important notes:
- Don’t introduce solids before 3 months adjusted age (even if your baby is 6 months chronological age) unless advised by a healthcare professional.1,2
- If your baby hasn’t met feeding readiness signs by 8–9 months chronological age, seek advice from your paediatrician or a feeding therapist.
- If your baby has developmental delays or medical needs, check with your healthcare team before starting solids
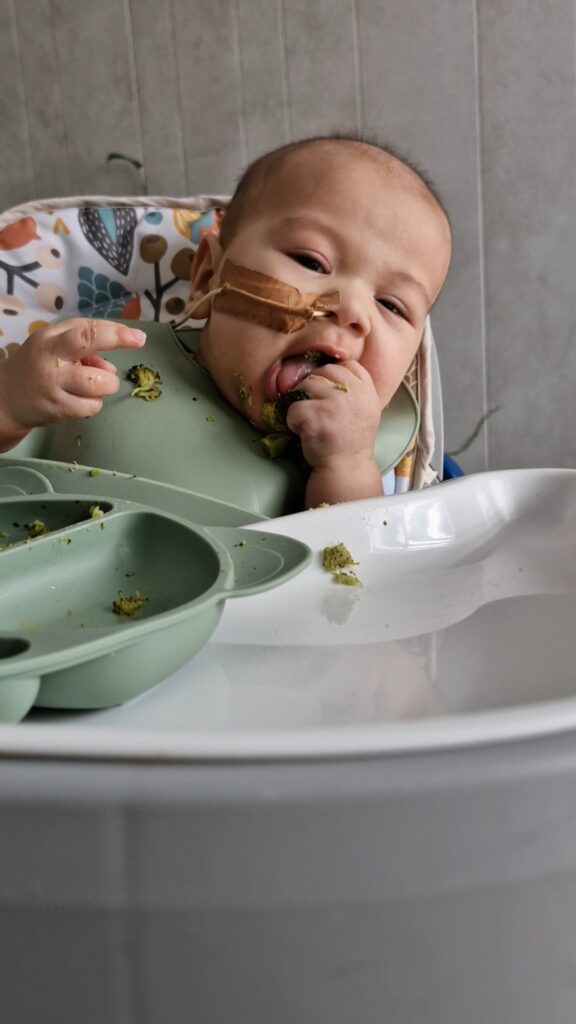
Baby not sitting upright?
To help your little one sit upright, you can place a rolled towel or small blanket behind their back/pelvis. This will help them shift their weight forward. To help your child evenly distribute their weight you can place a rolled towel on either side of their body.
To help your little one reach their tray, you can adjust the chair settings or boost their height by sitting them on a book or a few folded towels.
To help your child place their feet firmly on a footrest, you first want to ensure they are sitting upright and are evenly distributing their weight. Once this is achieved, you can focus on the footrest. Some high chairs have adjustable foot rest settings, while others may require purchasing a footrest add-on or using alternative items in your environment, but for other chairs you may need to purchase a foot rest or utilise something in your environment such as a dining chair, large box or a few books.
Read more about highchairs here.
What About Iron?
Most iron transfer from mother to baby happens in the final trimester of pregnancy. This means preterm babies often start life with lower iron stores. They’re also working hard on catch-up growth, which increases their iron requirements compared to term babies.3,4
Many babies born prematurely will have iron supplementation recommended by their paediatrician – this is typically recommended to continue until 12 months chronological age but we recommend that you clarify this with your treating team/feeding specialist/GP.
Note: Not all iron supplements are created equal – some forms are better absorbed and less likely to cause constipation or tummy discomfort. If you’re unsure which type is right for your baby, you can book a consultation with our dietitians in the Boob to Food online clinic. Our team can help you choose the most suitable option and create a plan with your paediatrician or GP for meeting your baby’s iron needs.
Iron-Rich Foods for Babies
When your baby is developmentally ready to start solids, iron-rich foods should be a priority – just as for term babies. Aim to include at least one source of iron at each meal.
Animal-based (haem iron – best absorbed):
- Liver (chicken, beef, lamb)
- Red meat (beef, lamb, kangaroo) – slow-cooked, minced or shredded
- Poultry (chicken, turkey) – particularly thigh and drumsticks
- Fish (salmon, sardines, mackerel, tuna)
- Eggs – especially the yolk
Plant-based (non-haem iron – less easily absorbed):
- Lentils (red, green, brown)
- Chickpeas, kidney beans, black beans, cannellini beans
- Tofu and tempeh
- Quinoa, amaranth, teff, buckwheat
- Pumpkin seeds (ground for babies)
- Tahini (sesame paste – spread thinly or mixed into purées)
- Dark leafy greens (spinach, silverbeet, kale)
Iron absorption tips:
- Pair plant-based iron sources with vitamin C-rich foods (tomato, citrus, berries, kiwi, broccoli, capsicum) to boost absorption.
- Avoid offering large amounts of dairy alongside iron-rich meals, as this can reduce absorption.
For recipe ideas that incorporate high-iron foods, check out our starting solids book Milk to Meals.

If Your Baby Has Additional Feeding Needs
Some preterm babies may face extra challenges such as:
- Tube feeding (NG or PEG)
- Reflux
- Oral aversion or sensory differences
- Developmental delays
- Medical conditions affecting body systems (e.g. cardiorespiratory, gastrointestinal, neurological, renal, immunological, vision)
In these cases, work closely with a paediatric feeding therapist, dietitian, occupational therapist or speech pathologist. Some support may be available through a GP management plan or NDIS if ongoing assistance is required.
Baby-Led Weaning or Puree for Premature Babies?
There’s no one-size-fits-all when it comes to how you start solids – especially if your baby was born early. Whether you begin with purées or follow a baby-led weaning (BLW) approach, the most important thing is to follow your baby’s cues and readiness signs.
Some premature babies may have slightly delayed motor skills (like head control, sitting stability, or hand-to-mouth coordination), which can make self-feeding a bit tricky at first.5 In these cases, starting with purées might feel like a gentler and more supported beginning – and that’s completely okay. Purées can still be responsive and baby-led when offered at your baby’s pace.
Other babies might show strong readiness signs closer to their adjusted age and may happily manage soft finger foods from the beginning. That’s okay too.
The key is not to rush and to remember that what works for one baby may not work for another. If your baby has:
- Motor delays (gross or oral motor),
- Reduced airway protection,
- Ongoing health concerns (like cardiorespiratory issues),
- Or if you’re feeling unsure or anxious about how to start…
…then it’s a great idea to check in with a paediatric feeding therapist, occupational therapist or speech pathologist. They can guide you with confidence and tailor a feeding plan that feels safe and achievable for you and your baby.
Feeding as a Sensory Experience
Feeding is not just about nutrition, it’s also sensory. Many preterm babies have had medical interventions like tubes or suctioning, which can make their mouths extra sensitive. Building positive sensory experiences around food helps babies learn that eating is safe and enjoyable.
Tips:
- Allow extra time for adjusting to new tastes, textures and temperatures. Encouraging exploration helps babies learn that eating is safe and enjoyable.
- Encouraging oral play with teethers, mouthing toys, and gentle gum massage can help prepare babies for solids.
- Keep mealtimes calm and predictable to reduce overwhelm.
- Watch your baby’s cues. Turning away, gagging, or pushing food out means slow down.
Texture progression: Some preterm babies may take longer to move through textures which can be completely normal. Reach out to a speech pathologist, feeding therapist or OT if your baby needs additional support.

Feeding Challenges
Being born early does increase the chance of feeding challenges later on, but it doesn’t mean your baby will definitely experience them.6,7 Many preterm babies go on to eat and grow without major difficulties. Still, it’s helpful for parents to be aware of a few things to look out for, so you can seek support early if needed.
Research shows that premature babies are more likely to:
- Take a little longer to adjust to new textures or tastes
- Show avoidant behaviours around food (like turning away or refusing)
- Need more support with motor skills that affect feeding (like sitting upright or bringing food to their mouth)
When to seek extra support:
- If you had prolonged difficulties with early feeding (breast/bottle) – it may be worth linking up with a feeding therapist early to support you in your journey to solids – for example if your baby is consistently coughing or spluttering during milkfeeds, or experiences recurrent chest infections.
- They show little interest in food after 6 weeks of repeated exposure
- Food falls straight out of their mouth with little control
- They show significant distress or avoidance at mealtimes
- By around 8 months, there is no sign of munching or chewing emerging
If you notice any of these signs – or if feeding simply feels harder than it should – it’s worth reaching out to a feeding therapist, speech pathologist or paediatrician. Early support can make feeding easier, safer, and more enjoyable for both you and your baby.
Remember: every baby’s journey is unique. Many preterm babies thrive with solids – and if challenges come up, there’s always help available.
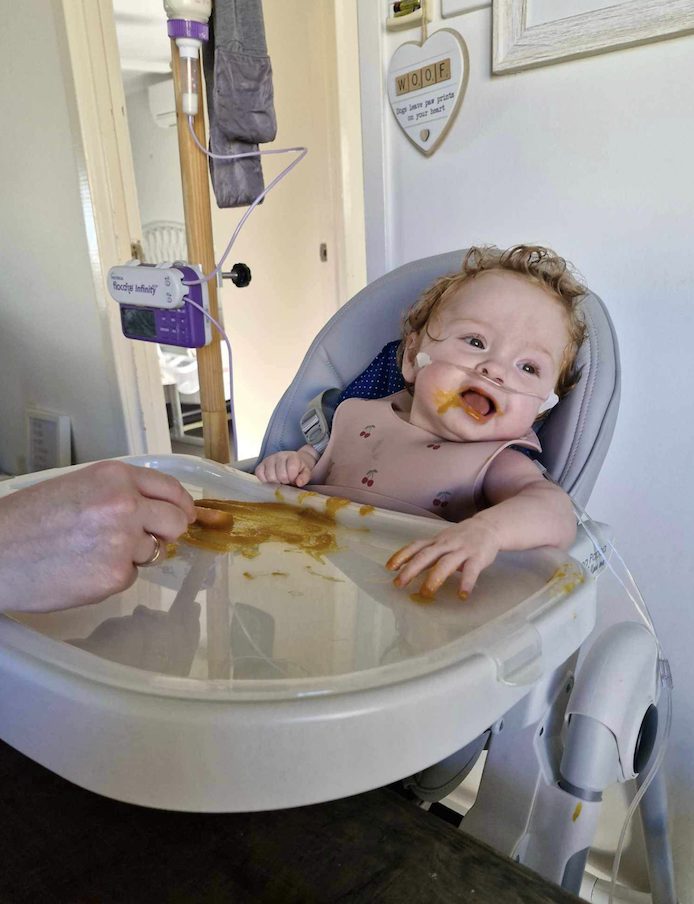
Other Common Concerns
Growth and weight gain:
Solids in the first year are meant to complement milk, not replace it. If weight gain is a concern, work closely with your paediatrician, dietitian, or IBCLC. Growth is usually plotted using corrected age until 24 months – which will often be reflected on the growth chart.
Allergen introduction:
The same principles apply as with term babies. When your baby is developmentally ready to start solids, early and ongoing exposure to allergens is recommended. Learn more about introducing allergens here.
Key Takeaways
- Use adjusted age (not just birth age) when tracking your baby’s development.
- Wait for all feeding readiness signs before offering solids.
- Prioritise iron-rich foods from the very beginning.
- Reach out for help early if feeding feels harder than it should.
References
- The Royal Women’s Hospital. Introducing solids to premature babies, 2019,https://www.thewomens.org.au/images/uploads/fact-sheets/Introducing-solids-to-premature-babies-200219.pdf.
- Palmer DJ, Makrides M. Introducing solid foods to preterm infants in developed countries. Ann Nutr Metab. 2012;60 Suppl 2:31-8. doi: 10.1159/000335336. Epub 2012 Apr 30. PMID: 22555187.
- Moreno-Fernandez J, Ochoa JJ, Latunde-Dada GO, Diaz-Castro J. Iron Deficiency and Iron Homeostasis in Low Birth Weight Preterm Infants: A Systematic Review. Nutrients. 2019 May 16;11(5):1090. doi: 10.3390/nu11051090. PMID: 31100900; PMCID: PMC6566715.
- Ferri C, Procianoy RS, Silveira RC. Prevalence and risk factors for Iron-Deficiency Anemia in very-low-birth-weight Preterm infants at 1 year of corrected age. J Trop Pediatr. 2013;60(1):53–60.
- Babble & Munch Learning. (2025). Circles to Feeding™ – Pediatric Program 2025. Retrieved August 25, 2025, from Babble & Munch Learning website
- Pados BF, Hill RR, Yamasaki JT, Litt JS, Lee CS. Prevalence of problematic feeding in young children born prematurely: a meta-analysis. BMC Pediatr. 2021 Mar 6;21(1):110. doi: 10.1186/s12887-021-02574-7. PMID: 33676453; PMCID: PMC7936467.
- Hee Chung E, Chou J, Brown KA. Neurodevelopmental outcomes of preterm infants: a recent literature review. Transl Pediatr. 2020 Feb;9(Suppl 1):S3-S8. doi: 10.21037/tp.2019.09.10. PMID: 32206579; PMCID: PMC7082240.

Back in stock
Toddler to Table now back in stock!
Your guide to bringing the family together, one meal (and delicious recipe) at a time.
Order now














Add a comment
Show Comments
0Leave a Comment
Your email address will not be published. Required fields are marked *