Tongue Ties
What should you do?
Contents

Back in stock
Toddler to Table now back in stock!
Your guide to bringing the family together, one meal (and delicious recipe) at a time.
Order nowTongue ties seem to be everywhere lately. And with that, everyone seems to have an opinion, a success story or a horror story. There is still a lot of confusion and ambiguity in the world of TOTs (tethered oral tissues). So the hope of this blog is to demystify it a little bit, extend a helping hand, and let you know how best to navigate the confusing world of ties and tethers.
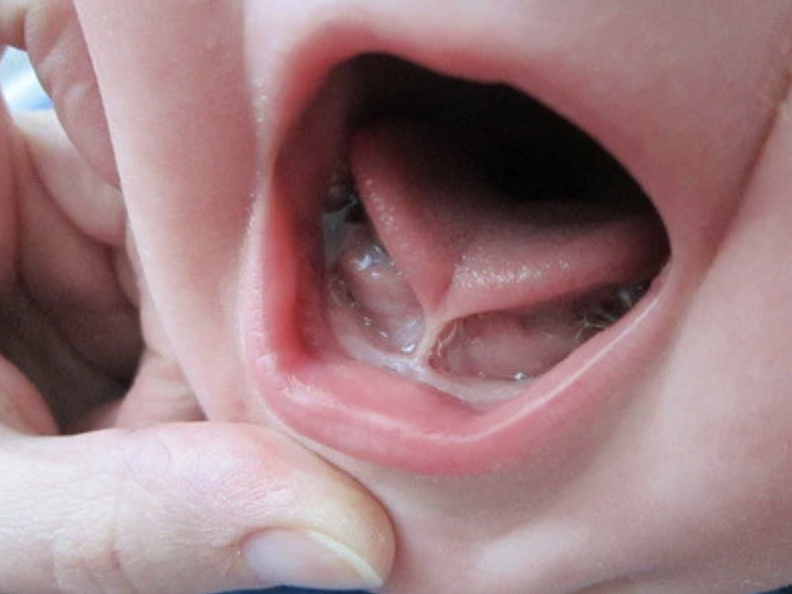
What is a tongue tie?
A tongue tie (ankyloglossia) is a common, often inherited condition present at birth where the thin piece of tissue (frenulum) connecting the underside of the tongue to the floor of the mouth is too short or tight; affecting the tongue movement and function. This can in turn impact your baby’s ability to feed – at the breast, via a bottle or with solid food.
Diagnosis
Sometimes, there may be early clues or signs that your little one could have a tongue tie prior to starting solids.
During early infant feeding, a number of feeding difficulties with both breast or bottle feeding may be attributed to a tongue tie. These include:1,2,3
- Poor latch
- Fatigue when feeding
- Consistent ‘cluster’ feeding; “marathon feeds” (constant/ very long feeds beyond the newborn period)
- Fussiness on the breast
- Poor weight gain
- Poor suction
- Clicking sounds
- Spillage/dribbling when feeding
Maternal symptoms include:4
- Nipple pain
- Breast engorgement, blocked ducts or mastitis
- Nipple damage
- Reduced breastmilk supply; especially if early supply was sufficient (this suggests that milk removal with feeds have not been sufficient to drive ongoing milk production)
We imagine that you’re probably looking at this list and thinking “well, that’s exactly what I experienced!” and this is where it gets tricky. Many of the reported difficulties could be attributed to tongue tie, but there could also be a plethora of other reasons that result in the difficulties encountered. This is where it’s essential that, if you do have concerns, you work with a lactation consultant or speech pathologist who is experienced in assessing tongue tie and you can get early diagnosis. Treatment options do differ based on the child’s age and this is where parents may hold some concerns.
Tongue ties and starting solids
While tongue ties are often identified during early milk feeds, some families don’t notice concerns until solids are introduced. Starting solids requires new oral motor skills, such as moving food side to side, chewing efficiently, forming a bolus and coordinating swallowing. If tongue movement is restricted, these skills can sometimes be more effortful.
If your baby has started solids, there are a number of things that you might notice if they have an undiagnosed or untreated tongue tie:5
• Slow or very effortful transition to solids
• Poor chewing efficiency or mashing food against the roof of the mouth instead of chewing
• Difficulty with swallowing
• Messy eating (food or liquid spilling out the front of the mouth)
• Gagging on lumps beyond what would be expected for their age
• Coughing or frequent spluttering during meals
• Difficulty progressing with straw or open cup drinking
• Very long mealtimes or early fatigue
• Ongoing poor weight gain
• Associated difficulty with certain speech sounds (in older babies and toddlers)
It’s important to remember that many of these signs can also be part of typical development, particularly in the early months of solids. Not every messy eater or child who gags has a tongue tie. However, if feeding feels consistently stressful, progress seems stalled, or your child is not meeting growth expectations, it’s worth seeking support from a speech pathologist, dietitian, lactation consult or GP.
Treatment
Treatment isn’t always straightforward. Infants under 6 months are typically offered a frenotomy – a quick procedure that involves snipping or lasering the frenulum . As babies get older, your specialist may suggest a frenectomy (removal of the frenulum) or frenuloplasty (frenectomy + typically repair with sutures). These are more complex procedures, which more commonly need to be performed under general anaesthetic.
Assessment and management of a possible tongue tie in an older baby may involve a care team including one or all of the following: GP, lactation consultant, speech pathologist, paediatric surgeon and/or paediatric dentist. Unfortunately not all health professionals are trained in recognising tongue tie and so you may need to ask around to ensure your concerns are being heard and you have complete trust in the knowledge and experience of your team.
A speech pathologist can help by conducting a feeding assessment (typically alongside a team including occupational therapist and dietitian), to determine whether the difficulties that you’re experiencing are age or developmentally appropriate, and from there will devise a treatment plan. Feeding therapy approaches are varied and very individualised to the child. In some cases, when the tethered tissue is not thought to be severe or the potential cause of feeding issues, significant improvements can be made through feeding therapy alone.
It’s important to know that we can’t diagnose a tongue tie based on the appearance of the tongue alone. If you’ve noticed that your little one has a more prominent or short frenulum but they’re not having any feeding issues, it’s often appropriate just to monitor. And there is still no evidence to suggest that tongue tie is linked to later speech or articulation difficulties either!6 So the old phrase of ‘if it ain’t broke, don’t fix it’ comes into play here. A number of studies have been conducted that have examined the influence of tongue tie revision on later speech and articulation difficulties and the results are very clear that preventative tongue tie revision is not advised.7 If there are issues and complications from the tie, then it might be the right option. But not in cases where parents are deciding to revise it ‘just in case’.
So what should you do?
If you suspect that your baby/toddler/child has a tongue tie that is impacting on their ability to feed and/or communicate, it’s worth partnering with an aligned team that hears your concerns. In infancy, this would be a lactation consultant, speech pathologist, specialist dentist or a discussion with your child health nurse or GP who can direct you to local services. For feeding concerns in toddlerhood and beyond, we recommend reaching out to a feeding team who may include occupational therapists, dietitians, speech pathologists and paediatricians.
References
- Brooks, L., Landry, A., Deshpande, A., Marchica, C., Cooley, A., & Raol, N. (2020). Posterior tongue tie, base of tongue movement, and pharyngeal dysphagia: what is the connection?. Dysphagia, 35(1), 129-132.
- Hill, R. R. (2021). Tongue-Tie: Prevalence, Significance, and Its Contribution to Maternal Feeding Challenges and Problematic Infant Feeding (Doctoral dissertation, Boston College).
- Cordray, H., Mahendran, G. N., Tey, C. S., Nemeth, J., Sutcliffe, A., Ingram, J., & Raol, N. (2023). Severity and prevalence of ankyloglossia-associated breastfeeding symptoms: A systematic review and meta-analysis. Acta Paediatrica. https://doi.org/10.1111/apa.16609
- Hill, R. R. (2021). Tongue-Tie: Prevalence, Significance, and Its Contribution to Maternal Feeding Challenges and Problematic Infant Feeding (Doctoral dissertation, Boston College).
- Sexton, M. (2018). Feeding behaviors and the child with posterior tongue-tie: comparison to norms. Electronic Theses and Dissertations. Paper 2925. https://doi.org/10.18297/etd/2925
- Webb, A., Hao, W., & Hong, P. (2013). The effect of tongue-tie division on breastfeeding and speech articulation: A systematic review. International Journal of Pediatric Otorhinolaryngology, 77(5), 635-646.
- Salt, H., Claessen, M., Johnston, T., & Smart, S. (2020). Speech Production in Young Children with Tongue-Tie. International Journal of Pediatric Otorhinolaryngology. https://doi.org/10.1016/j.ijporl.2020.110035

Back in stock
Toddler to Table now back in stock!
Your guide to bringing the family together, one meal (and delicious recipe) at a time.
Order now













Add a comment
Show Comments
0Leave a Comment
Your email address will not be published. Required fields are marked *